Systemising an allied health practice means documenting how patients flow through your clinic, from first contact to ongoing care, so your therapists can focus on clinical work instead of chasing admin. I've helped allied health clinics do this. The practices that get it right stop losing therapists to burnout and start building something that delivers consistent care without the founder in every treatment room.
If you're running a physio, OT, speech, chiro, or multi-disciplinary practice and you're spending more time on admin than on patients, this guide is for you.
Why allied health practice owners get stuck
You became a clinician because you wanted to help people. Somewhere along the way, you became a business owner instead.
Now you're managing rosters, chasing referrals, handling NDIS paperwork, reviewing invoices, training new therapists, dealing with cancellations, and somehow still trying to see your own patients. The clinical work that brought you into this profession gets squeezed into whatever time is left after the admin.
Here's the pattern. You're good at what you do. Patients love you. Referrals come. You hire therapists. Then more. Now you're managing a team, but the knowledge of how your clinic should run, the standards, the patient experience, the way you want things done, it's all in your head.
Your therapists are clinically competent. But they don't know how you want the phone answered, how you want new patients onboarded, how invoices should be processed, or how to handle a complex NDIS plan review. So they either guess or they ask you. And you're back in the middle of everything.
Every allied health practice hits the same bottlenecks:
- Patient onboarding is inconsistent. One therapist does a thorough intake. Another rushes it. The patient experience depends on who they see, not on your clinic's standard.
- Admin eats clinical time. Invoicing, NDIS claims, report writing, scheduling. Your therapists spend hours on paperwork that could be streamlined.
- New therapists take months to get productive. Because "training" means shadowing a senior therapist and figuring out the admin on their own.
- Knowledge walks out the door. When a therapist leaves, their patient relationships and clinical knowledge leave with them. Nothing is documented.
- You can't step back. The practice depends on you being there. A week off means problems pile up.
The 90% invoicing reduction
Renee and Matt Kelly run Lime Therapy in Mildura, Australia. Multi-disciplinary allied health: OT, physio, speech therapy, hand therapy. Over 40 staff.
Renee is a big-picture thinker. She'd built a successful practice, but it was running on energy and effort rather than systems. They'd invested heavily in policies, but the policies sat in a folder. Nobody used them because they were compliance documents, not practical how-to guides.
The turning point came when they enrolled in the Systems Champion Academy and appointed Kaleb Grant as their Systems Champion. Kaleb wasn't a manager. He was a young occupational therapist, two years out of university. But he was organised, curious, and not afraid to ask "why do we do it this way?"
Kaleb interviewed therapists. He watched how the work was actually done. He documented the processes that were causing the most pain. And he started with the one that was eating the most time: invoicing.
The result: invoicing time reduced by 90%.
Not 10%. Not 20%. Ninety percent. A process that had been consuming hours of therapist time every week was systemised to the point where it barely took any time at all.
But the real transformation was cultural. SYSTEMology became part of the company language. Team members started proactively looking for systemisation opportunities. They weren't just following systems. They were building them.
The Critical Client Flow for allied health
The Critical Client Flow maps the patient journey through your practice. For allied health, it typically follows these stages:
- Referral or inquiry. GP referral, self-referral, NDIS plan manager, word of mouth.
- Initial contact. Phone call or online booking. Capture patient details, funding source, needs.
- Assessment and intake. First appointment. Clinical assessment, goal setting, treatment plan.
- Treatment delivery. Ongoing sessions. Progress tracking, clinical notes, plan reviews.
- Reporting and claims. Progress reports, NDIS reports, invoicing, insurance claims.
- Discharge or transition. Treatment completion, referral to another service, or transition to maintenance.
- Follow-up and re-engagement. Check-in after discharge, recall for annual reviews, referral back to GP.
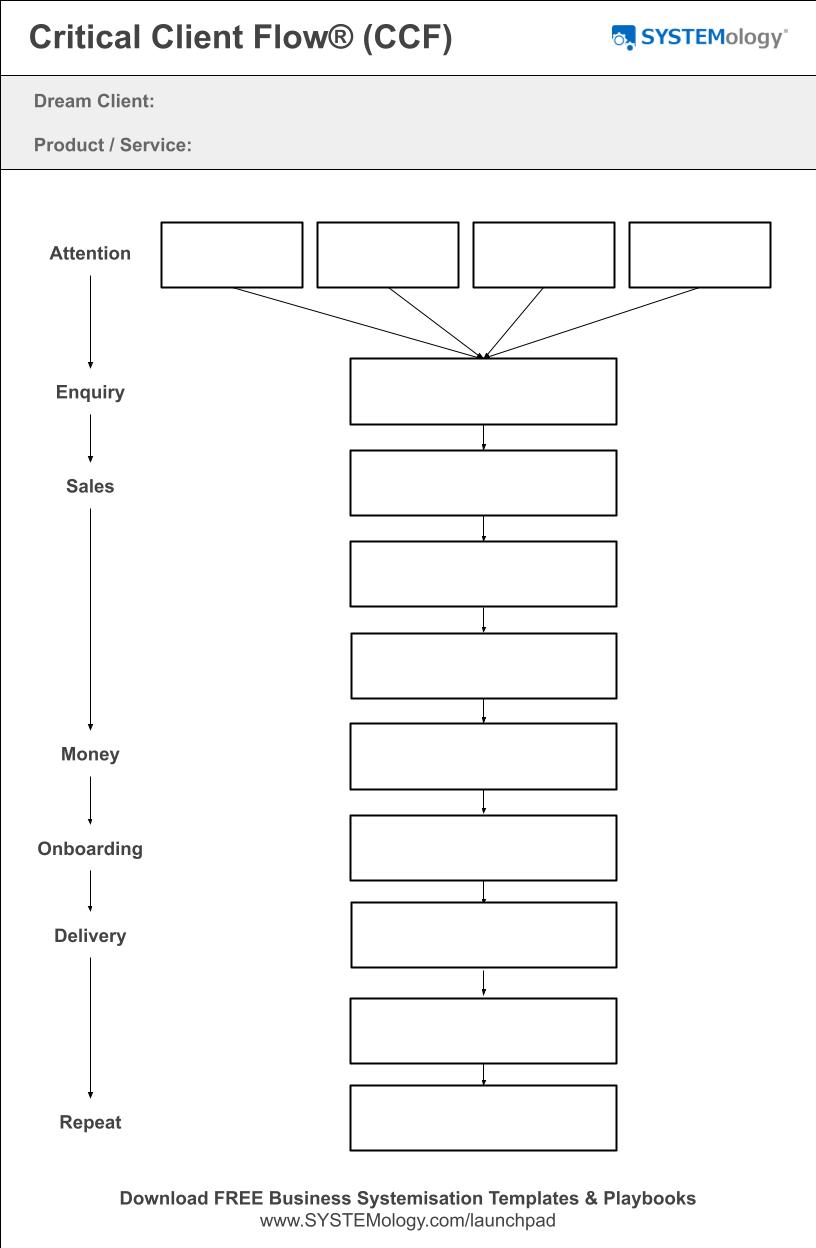
One key challenge in allied health: the patient journey blurs traditional department lines. Is booking a patient "sales" or "operations"? Is writing a progress report "delivery" or "admin"? The answer: classify based on which team performs the task, not the function it serves. Don't overthink the categories. Map the flow.
Another challenge unique to health practices: funding models create complexity. An NDIS patient journey looks different from a private patient journey, which looks different from a WorkCover claim. You may need to map your CCF for your most common funding type first, then adapt for others.
How to start systemising your allied health practice
Step 1: Map your Critical Client Flow
Write out the seven stages above for your most common patient type. Walk through each and ask: is this consistent? Does every patient get the same experience? Or does it depend on which therapist they see?
Most practices discover that their clinical delivery (stage 4) is reasonably consistent because clinical training ensures that. But everything around it, intake, admin, reporting, follow-up, is completely ad hoc.
Step 2: Appoint a Systems Champion
This is the lesson from Lime Therapy that matters most. Kaleb was a junior OT. Not a manager. Not the most experienced therapist. But he had the right mindset: organised, curious, willing to question how things had always been done.
Your Systems Champion needs dedicated time and authority. Not "do this on top of your patient load." Actual time carved out of their week to lead the documentation process. Renee and Matt gave Kaleb that time, and it was the single most important decision they made.
Step 3: Document the three systems costing you the most
For allied health practices, the top three are almost always:
Patient onboarding (first appointment). How a new patient goes from first contact to first session. What information is gathered, how they're set up in the system, what they're told to expect, who contacts them and when. When this is inconsistent, patients start with confusion and therapists waste time chasing missing details.
Invoicing and claims processing. How sessions get invoiced, how NDIS claims are submitted, how private health fund claims are processed. This is where Lime Therapy found their 90% reduction. The process was happening dozens of times a day, and every minute saved per invoice multiplied across the entire practice.
New therapist onboarding. How a new hire goes from day one to seeing patients independently. When this is in someone's head, it takes months. When it's documented, it takes weeks. In an industry with high turnover, this system pays for itself repeatedly.
Step 4: Put it in one central place
Your systems need to be accessible from any treatment room, any device. Not in a policies folder nobody opens. Not in someone's email. systemHUB is purpose-built for this and used by hundreds of health practices. But whatever you choose, one central location that your whole team checks first.

Learn more →
More practices making the shift
Sleep Right Australia provides personalised CPAP services for sleep apnea patients. Medical equipment, patient care, strict compliance requirements. They documented their processes in systemHUB: patient onboarding, equipment setup, follow-up care, inventory management. The result: consistent patient care, streamlined staff training, and a scalable foundation for new locations.
TECHealth operates in emergency room environments. If you can systemise an ER, you can systemise any health practice. They documented service delivery, technology implementation, and client support processes, creating a level of safety and reliability that the environment demands.
Body in Context is a medical massage clinic where insurance payment comes after service delivery, not before. They adapted the CCF framework to account for delayed payment and third-party payers, showing that the framework flexes to fit even unusual healthcare payment models.
These practices span allied health, medical equipment, emergency services, and clinical massage. Different specialisations. Same framework. Same result: the founder got their time back without clinical quality dropping.
And it's not just health practices. The same framework works for construction businesses, plumbing companies, accounting firms, and digital agencies.
What about AI in allied health?
AI is already changing healthcare administration. Automated appointment reminders, AI-assisted clinical note drafting, smart scheduling that reduces gaps and cancellations.
But the principle holds: process first, then AI.
AI can draft progress reports from session notes. It can auto-categorise NDIS line items. It can flag patients who haven't been seen in 90 days. But it can only do these things well if you've first documented what "good" looks like for your practice.
Lime Therapy's 90% invoicing reduction wasn't AI. It was a documented process that removed unnecessary steps. AI would make it even faster, but only because the process was already clean.
The bottom line
Allied health practices exist to help people. Every hour a therapist spends on admin is an hour they're not spending with a patient. Every inconsistency in your patient onboarding is a patient who starts their journey confused. Every undocumented process is knowledge that leaves when a therapist does.
Here's what it takes to fix it:
- Map your Critical Client Flow (the seven stages).
- Appoint a Systems Champion (it doesn't have to be your most senior therapist).
- Document the three systems costing you the most time.
- Put it all in one place your team can access from any treatment room.
Lime Therapy did it and cut invoicing time by 90%. Their team now proactively builds systems. Kaleb, a junior OT, became the person who transformed a 40-person practice.
If you're ready to see what that looks like for your practice, book a free Good Fit call and we'll map it out together.
Not ready for a call? Start with the full SYSTEMology framework and see how the method works.